Page 7 - SMU Spring 2020
P. 7
Surgical treatment with periacetabular
osteotomy (PAO) is the accepted treatment
for hip dysplasia with a lateral center
edge angle less than 20 degrees. In the
challenging competitive dance population,
over 80 percent have radiographic dysplasia
or borderline dysplasia (LCEA <25). 12
Multiple clinical series report long standing
symptom relief and return to previous
activity levels when hip dysplasia is treated
with PAO. 20,21 Return to sport is a concern
after any major orthopaedic procedure.
After PAO, 80 percent of recreational and
competitive athletes return to their sport
at a median 9 months after surgery and
73 percent return to the same level, though
this was less common in competitive
athletes (58 percent). In dancers,
22
63 percent will return by an average of
8.8 months after surgery. Periacetabular
10
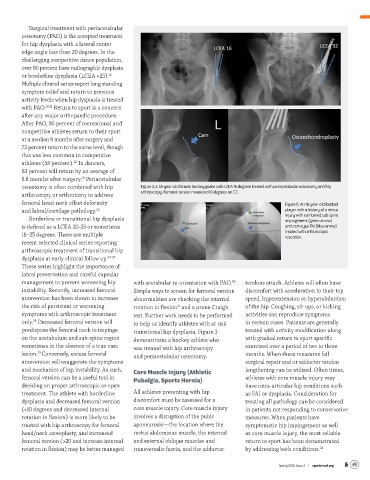
osteotomy is often combined with hip Figure 3, 4: 18-year-old female hockey goalie with LCEA 16 degrees treated with periacetabular osteotomy and hip
arthroscopy or arthrotomy to address arthroscopy. Femoral version measured 10 degrees on CT.
femoral head-neck offset deformity Figure 5: An 18-year-old football
and labral/cartilage pathology. 23 player with a history of a rectus
Borderline or transitional hip dysplasia injury with combined sub spine
impingement (green arrow)
is defined as a LCEA 20-25 or sometimes and cam-type FAI (blue arrow)
18–25 degrees. There are multiple treated with arthroscopic
resection.
recent selected clinical series reporting
arthroscopic treatment of transitional hip
dysplasia at early clinical follow up. 24-27
These series highlight the importance of
labral preservation and careful capsular
management to prevent worsening hip with acetabular re-orientation with PAO. tendons attach. Athletes will often have
30
instability. Recently, increased femoral Simple ways to screen for femoral version discomfort with acceleration to their top
anteversion has been shown to increase abnormalities are checking the internal speed, hyperextension or hyperabduction
the risk of persistent or worsening rotation in flexion and a prone Craig’s of the hip. Coughing, sit-ups, or kicking
31
symptoms with arthroscopic treatment test. Further work needs to be performed activities can reproduce symptoms
only. Decreased femoral version will to help us identify athletes with at risk in certain cases. Patients are generally
28
predispose the femoral neck to impinge transitional hip dysplasia. Figure 3 treated with activity modification along
on the acetabulum and sub-spine region demonstrates a hockey athlete who with gradual return to sport specific
sometimes in the absence of a true cam was treated with hip arthroscopy exercised over a period of two to three
lesion. Conversely, excess femoral and periacetabular osteotomy. months. When these measures fail
29
anteversion will exaggerate the symptoms surgical repair and or adductor tendon
and mechanics of hip instability. As such, Core Muscle Injury (Athletic lengthening can be utilized. Often times,
femoral version can be a useful tool in Pubalgia, Sports Hernia) athletes with core muscle injury may
deciding on proper arthroscopic or open have intra-articular hip conditions such
treatment. The athlete with borderline All athletes presenting with hip as FAI or dysplasia. Consideration for
dysplasia and decreased femoral version discomfort must be assessed for a treating all pathology can be considered
(<10 degrees and decreased internal core muscle injury. Core muscle injury in patients not responding to conservative
rotation in flexion) is more likely to be involves a disruption of the pubic measures. When patients have
treated with hip arthroscopy for femoral aponeurosis—the location where the symptomatic hip impingement as well
head/neck osteoplasty, and increased rectus abdominus muscle, the internal as core muscle injury, the most reliable
femoral version (>20 and increase internal and external oblique muscles and return to sport has been demonstrated
32
rotation in flexion) may be better managed transversalis fascia, and the adductor by addressing both conditions.
Spring 2020, Issue 2 | sportsmed.org 5